Voice dictation to improve the inpatient nurse workflow


Nuance had previously ran a study with a previous research group from Bentley University from this course that focused on the physician/patient experience and interaction. They now wanted to look at nurses and how they collected data. They had some basic knowledge on nurses and their use of paper and flowsheets informed by preliminary research but they wanted to examine their current assumptions by seeing what was happening in the field.
The major milestones we hit included goal setting and alignment, nurse interviews, coding and insight generation, as well as a workshop we ran with stakeholders.
Working with our stakeholders at Nuance, our team outlined 4 goals for the project that we would try to attain with our research:
5 researchers from Bentley University, including myself. Our team partnered with Nuance Communications, a healthcare technology company. From their team, we worked directly with the Principal UX designer and Senior UX researcher. I was responsible for running interviews, qualitative coding, thematic analysis, and developing several sections of the report.
We used various methodologies including semi-structured remote interviews, questionnaires, and a round-robin ideation session. We conducted semi-structured interviews with ten nurses working in high-acuity inpatient settings, to learn more about nurses' motivations, patient data collection workflows, and associated challenges.
Due to constraints due to the COVID-19 pandemic, the logistic hurdles of direct observation in hospitals, and time, our team agreed that semi-structured remote interviews would be an appropriate method for this research.
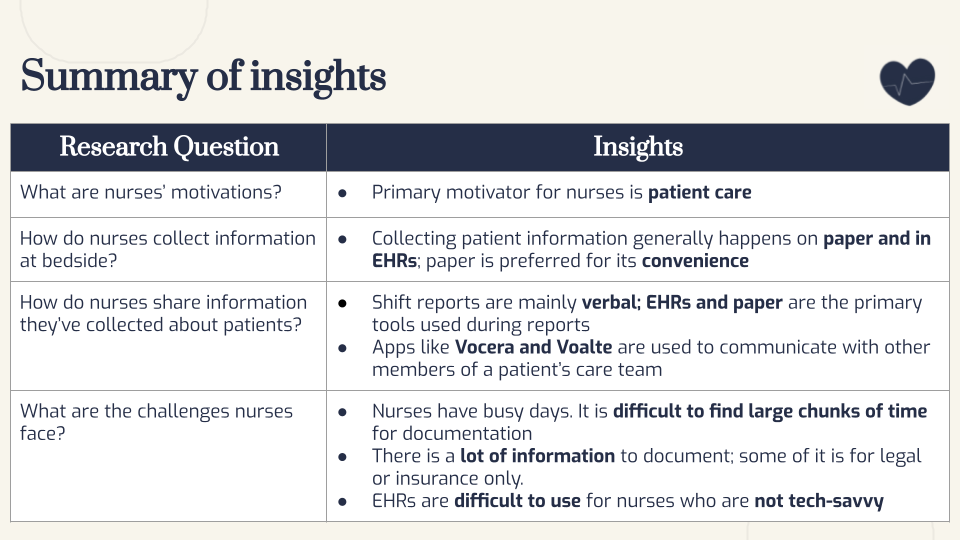
Multiple rounds of thematic analysis led to several high-priority insights:
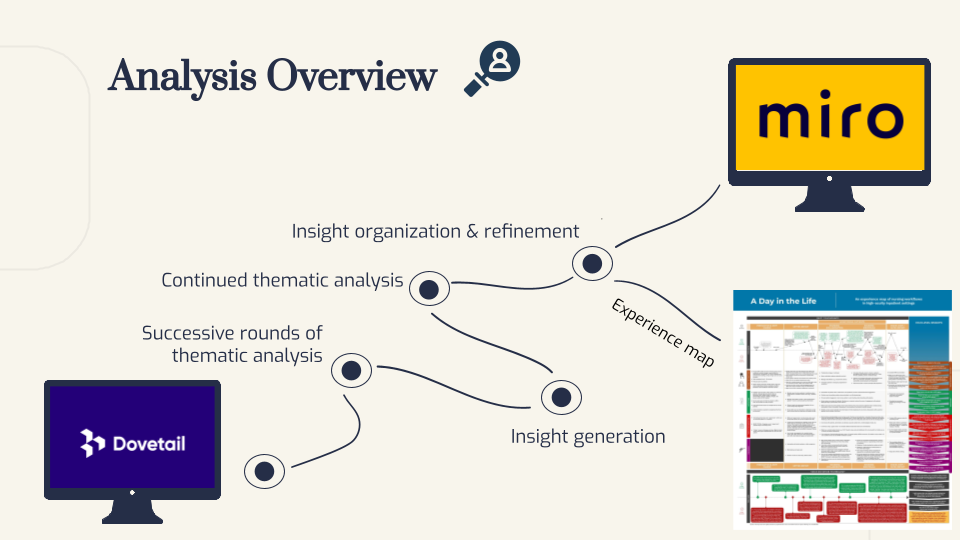
After understanding current data collection workflows through the interviews, our goal was to explore whether these workflows might be improved through voice technology. We developed three artifacts to aid this effort:
Our research showed that despite the time-consuming demands of patient documentation and the use of telecommunication devices, a majority of nurses did not favor the idea of using voice dictation when it came to documenting patient data. However, voice technology is more than just voice dictation, and our final recommendations on the use of voice technology for nurses in inpatient settings are as follows: